

Dr. Palash Gupta (Sr. Consultant), MBBS, MS (Orthopedics), Fellowship in Arthroplasty (Knee & Hip), Fellowship in Arthroplasty & Trauma, Unit Head & Senior Consultant Joint Replacement & Orthopedics, Sri Balaji Action Medical Institute, 25+ years of Experience Are you burdened by the constant agony of knee pain, making even the simplest tasks feel like a herculean effort? If you reside in Rohini and seek a solution to your knee troubles, Dr. Palash Gupta, a renowned Total Knee Replacement Surgeon, is here to offer you relief and a renewed lease on life.
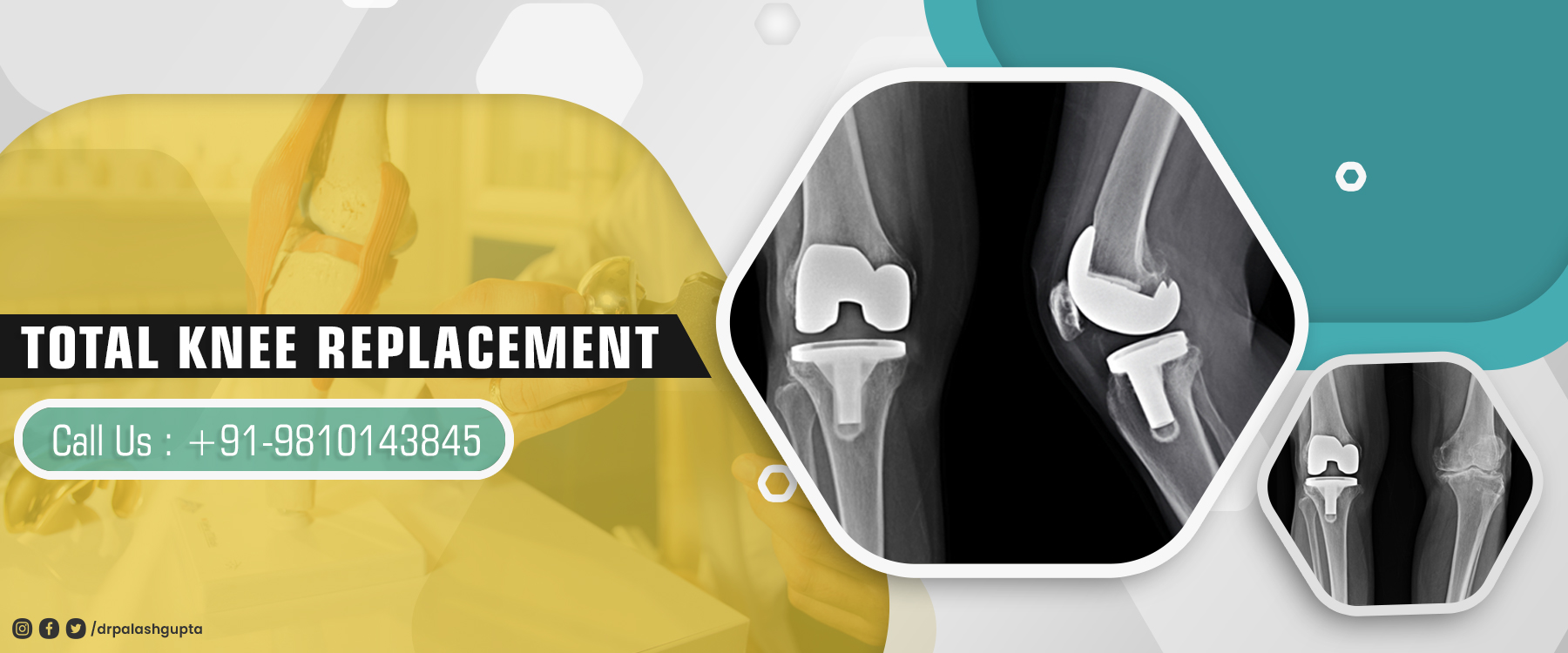
Total Knee Replacement (TKR), also known as knee arthroplasty, is a surgical procedure designed to alleviate pain and restore function to severely damaged knee joints. It holds the power to transform the lives of those suffering from conditions like osteoarthritis, rheumatoid arthritis, or traumatic injuries.

Imagine a life free from the shackles of persistent knee pain, where you can walk, climb stairs, and engage in activities you cherish without hindrance. Dr. Palash Gupta specializes in providing this transformation, and his commitment to enhancing your overall well-being is unwavering.
Your Journey to Freedom from Knee Pain - Opting for total knee replacement surgery is a significant decision, and Dr. Palash Gupta is here to guide you through every step. Here's what you can anticipate when you choose him as your Total Knee Replacement Surgeon in Rohini:
Your New Beginning Starts Here Bid farewell to debilitating knee pain and reclaim your life. Dr. Palash Gupta invites you to take the first step toward a pain-free future. Envision a life where you can walk, run, and engage in activities you adore without hesitation.
Contact Dr. Palash Gupta Today! The path to a pain-free life is within your grasp. Reach out to Dr. Palash Gupta, the leading Total Knee Replacement Surgeon in Rohini, and embark on your journey toward renewed mobility and an improved quality of life. Don't let knee pain define your future; take control and embrace a healthier, happier you.
Treatments Offered
Total Knee Replacement Surgeon
BEFORE THE SURGERY What tests and precautions are required before planning a knee replacement surgery? It is important to have good quality X-rays of the knee.
Read More +Components of a total knee replacement A total knee replacement prosthesis has four components: femoral component (made of metal) which is fixed to the cut.
Read More +What is total knee replacement (TKR)? It is also known as total knee arthroplasty (TKA). Knee replacement surgery involves replacing the worn out (diseased and painful).
Read More +Hip Joint Replacement is a surgical procedure that relieves pain from most kinds of hip arthritis, improving the quality of life for the large majority of patients.
Read More +Shoulder joint replacement surgery (also called shoulder arthroplasty) is not as common as replacement surgeries for the knee or hip joints. Still, when necessary.
Read More +Elbow joint replacement (also called elbow arthroplasty) can effectively treat the problems caused by arthritis of the elbow. The procedure is also becoming more widely.
Read More +
Book An Appointment
Why Choose Us
Dr. Palash Gupta has excellent academic record and admirable working experience at national and international level. He brings his vast experience to India on a full time basis and has gathered a team of professionals whose sole purpose is to facilitate the patient’s journey to freedom from joint pain. He is also actively involved in teaching under-graduate medical students as well as post-graduate orthopedic residents. Dr Palash Gupta is an active faculty member for a number of national and international conferences on Arthroscopic Surgery and Joint Replacement. The glimpse of his experience is as follows:



Specialized Doctor Details
Dr. Palash
Orthopedic SurgeonDr. Palash Gupta has excellent academic record and admirable working experience at national and international level. He brings his vast experience to India on a full time basis and has gathered a team of professionals whose sole purpose is to facilitate the patient’s journey to freedom from joint pain. He is also actively involved in teaching under-graduate medical students as well as post-graduate orthopedic residents. Dr Palash Gupta is an active faculty member for a number of national and international conferences on Arthroscopic Surgery and Joint Replacement. The glimpse of his experience is as follows:
Ophthalmology Prize for securing 1st rank in Obs. & Gynaecology
What Clients Say


Copyright © Knee Joints Replacement 2023. All rights reserved. | Designed & Developed by : Global Ad Media